The Space Between Fitness and Medicine: Where “the Good You Do For Others” Brings the Reward you Deserve | Part 2
In our first part of this three-part discussion, in addressing the topic of financial reward, I asked you to ponder the value of restoration. What, I prompted you to consider, is the value of helping someone who has moved along the dis-ease continuum, gradually leaving health in the proverbial rear-view-mirror back toward divine health?
 It isn’t an easy question to answer. We can tackle it by considering all of the dollars those who incur inflammatory issues, chronic challenges, and cellular degradation will have to invest in maintaining function and comfort. We might also attempt to place a monetary value upon lost quality of life. We might even consider the simple question, “what would someone pay to rediscover health” considering their fear and apprehension of the alternative, and from that extrapolate the value.
It isn’t an easy question to answer. We can tackle it by considering all of the dollars those who incur inflammatory issues, chronic challenges, and cellular degradation will have to invest in maintaining function and comfort. We might also attempt to place a monetary value upon lost quality of life. We might even consider the simple question, “what would someone pay to rediscover health” considering their fear and apprehension of the alternative, and from that extrapolate the value.
If you are willing to believe that personal trainers with advanced education and the development of a complementary skill set can have immeasurable impact upon “the unwell population,” one perspective becomes clear.
The trainer versed in restoring health commands a far greater value than the personal training mainstream.
That’s important.
STEPPING UP A LEVEL
As in any field, a specialist with enhanced value will serve his or her marketplace best by finding a direct line of contact with those in need of their specialty.
In the sentence above, “need” is the key word.
While it’s oft been said that personal trainers are a luxury or a privilege, with an appropriate adjustment in perspective, those who have slipped into the largest segment of our adult population, the unwell market, might consider any therapeutic resource, if wellness is a goal, a “need.”
Now that I’ve mentioned it a few times, I’ll provide a general description of the market I’m referring to as “unwell.” Then I’ll help you see the opportunity to step up, to meet this population in an arena where they “need” you. I’, to command a value in line with a well-justified fee, and . . . here’s the biggie . . . to provide them the service they will truly benefit from.
WHO ARE THE UNWELL?
Let’s be really clear here. I’m not suggesting the opportunity lies in training “sick people.” I’m suggesting the largest, most opportune market share is made up of many American adults between the ages of 35 and 65. They aren’t “sick” in a clinical sense. They work. They drive their kids to school. They shop in the malls and grocery stores. They eat in the neighborhood restaurants. They pump gas in the same gas stations you do and they frequent Starbuck’s, Chipotle, and the local pizza place.
They don’t have need for hospitalization or chronic care . . . but they’ve slipped, moved along what I’m calling the dis-ease continuum. They’ve begun a process of maladaptation, a movement away from healthful homeostasis, and while many haven’t yet been diagnosed (many have), their bodies have become imbalanced. Whether it’s a hormonal imbalance, thyroid irregularity, blood sugar elevation, hypertensive condition, hypercholesterolemia, or chronic inflammation of one or several bodily systems, they have moved into a place where innate homeostasis is no longer their “norm.”
Not sick, at least not clinically, but not well. What’s alarming is, I’m describing near 65% of the adult population over the age of 45. Yes, the market is vast.
If the unwell were being cured of their ailments or remedied by the conventions of medicine, I wouldn’t see the “need” as being this opportune. All I need to share is a single statement to help you see why there’s a desperate need for a new type of health practitioner, one who masters the exercise and eating intervention. Here’s that statement.
In a society where chronic disease is most treated with pharmaceutical intervention, there isn’t a single medication that will cure any chronic disease.
Read that again. While there exists a wild array of meds to manage conditions and change biomarkers, there isn’t one that will cure the plight of the unwell.
Conversely, there is an extensive body of evidence to demonstrate the power we have over shifts in blood sugar, blood pressure, and hormonal disruption when we strategically employ a variety of exercise modalities and guidance in the realm of supportive nutrition.
If the demand is great, the “need” remains unfulfilled, and the greatest potential lies in the skill set we, as fitness professionals, have access to . . . our value escalates above virtually any conventional yet impotent “cures.”
THE LEVEL 2 TRAINER AS A CORRECTIVE HEALTH SPECIALIST
If we consider a “Level 1” trainer someone who is qualified, credentialed, and able to provide safe and effective exercise prescription to a healthy population, let’s consider a “Level 2” someone who can effectively target this Unwell niche and deliver improvements in biomarkers, condition, and quality of life.
The Level 2 trainer can identify his or her “ideal client avatar.” Moving forward I’ll refer to the Ideal Client Avatar as an “ICA.”
In establishing a presence and a track record with the Unwell, the enhanced personal trainer (enhanced with a higher level of education than the standard and an ability to implement positive change in the unwell) can justifiably command fees in line with other health practitioners, medical practitioners, and specialists.
In setting a fee structure, there should be a professional standard, a relationship-based fee that is consistent, one that exceeds “an industry standard.” Remember, if you deliver above the standard, you deserve reward above the usual.
 HOW DO YOU STEP UP AND CREATE AN AUDIENCE?
HOW DO YOU STEP UP AND CREATE AN AUDIENCE?
Marketing, for the Level 2 trainer targeting this niche is not as haphazard as “pass out cards, talk it up in the gym, and talk to everyone about what you do.”
In order to establish your position, you’ll want to have four. Four strong successes. Four living examples of the value you deliver, and finding those four requires a bit of front-end work. Once you have your four you have a sound foundation upon which to build. The question, therefore, that merits consideration is . . . how do you “break in.” Where do your “four” come from.
I’ll make it step by step.
Note that everything that follows is based upon the assumption that you have received extraordinary training, that you’ve established a level of education complementary to your base credential, and that you’re positioned to initiate and maintain a practice with a revised focus on empowering clients to reverse the imbalances inherent in chronic disease. This is a prerequisite of paramount importance and although I won’t invest any more time in addressing it here, don’t allow my failure to repeat and reiterate this point as an indication its any less than vital.
STEP ONE: Define your Ideal Client Avatar. If you have a personal connection to a given condition or population (i.e. a relative with diabetes, a personal history with thyroid issues, etc.) and you have a passion for helping others who you feel are kindred spirits, that’s where you should best direct your marketing. You can’t “market well” until you define your ICA. This is a “must” in turning your ambition into financial security (and it’s the step most who seek to elevate their careers miss or ignore). Your ICA may not be based on your personal experience, but rather on where you see the greatest opportunity or where you have the greatest inroads. Devote time to getting clear on your ICA. It’s the true key to successfully “Stepping up to Level 2.”
STEP TWO: Determine your fee structure, your promise, and your offer. You don’t want to approach each prospective client with an open negotiation, nor do you want to exhibit uncertainty. As any business owner, design your foundation. What, precisely, are you promising each client? How are you compensated for that? What, precisely, is the person considering retaining you, supposed to do now, as a point of commitment.
STEP THREE: Choose a location, an affiliation, a network, and a social media platform where you can “meet” your ICA and spread the word. This is far simpler than it sounds. In outlining your ICA, simply as the question, “where do I find him (her)?” This is marketing at its core. Don’t think “medical.” Think real life. Where can you do a talk, a workshop, a presentation, knowing your ICA sits in the audience. I realize this is the intimidating step . . . but it’s also the one that brings you to human connection, and ultimately to commitment and money exchange. Perhaps in the future I’ll share an entire article devoted to “finding your ICA in the real world.” For now, accept that you have the answer to the question, you have the ability, and all it takes is a bit of courage and determination.
STEP FOUR: Create your Four. Do your thing. Work your magic. Use your skill set. Bring about change. Documentable change. Once you have your first four successes, you begin to build what I call an Arsenal of Evidence, and from that point on, the marketing challenge is replaced by magnetic appeal.
STEP FIVE: Build your business confidently, massively, professionally, and without limit.
This 3-part piece is intended, not to be a complete primer for business building, but to give you a sense of both the opportunity and your ability.
In creating a distinction between the progressive trainer willing to study, learn, and elevate, I’ve used the term “Level 2,” not to suggest any elite status, but to demonstrate a clear escalation in earning potential. Before I conclude this second part of the piece, I’ll outline a few elements of what I’m calling The Level 2 Trainer.
FIVE DISTINCTIVE ELEMENTS OF THE LEVEL 2 TRAINER
- You are a specialist among a given population
- You command fees above the norm
- You have a consistent promise and offer
- You have a track record and consistently grow a marketing / referral base
- You understand and recognize the value in the potential you have as a guide to empower others to move away from chronic disease and back toward divine health
Is there a level above the Level 2 trainer? Yes. And the sky’s the limit. Literally. More to come in Part 3!
This is 3 part series. Read part 1 here, and part 3 here
Phil Kaplan has been a fitness leader and Personal Trainer for over 30 years having traveled the world sharing strategies for human betterment. He has pioneered exercise and eating interventions documented as having consistent and massive impact in battling chronic disease. His dual passion combines helping those who desire betterment and helping health professionals discover their potential. Email him at phil@philkaplan.com


 The professions that require a state or national licensures, such as physicians, nurses, or physical therapists, help to provide checks and balances on who should and should not be providing a service to any individual. However, there are many professions within our healthcare community that are poorly understood and many times misrepresented by individuals with minimal certifications or credentials.
The professions that require a state or national licensures, such as physicians, nurses, or physical therapists, help to provide checks and balances on who should and should not be providing a service to any individual. However, there are many professions within our healthcare community that are poorly understood and many times misrepresented by individuals with minimal certifications or credentials.








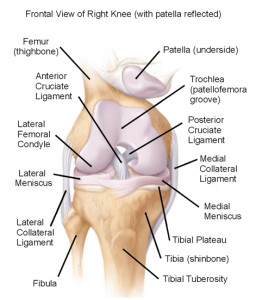
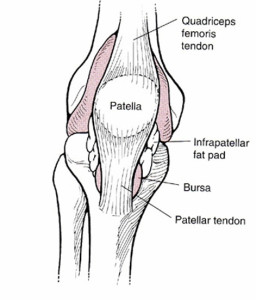




 Chris is the CEO of Pinnacle Training & Consulting Systems (PTCS). A continuing education company, that provides educational material in the forms of home study courses, live seminars, DVDs, webinars, articles and min books teaching in-depth, the foundation science, functional assessments and practical application behind Human Movement, that is evidenced based. Chris is both a dynamic physical therapist with 14 years experience, and a personal trainer with 17 years experience, with advanced training, has created over 10 courses, is an experienced international fitness presenter, writes for various websites and international publications, consults and teaches seminars on human movement. For more information, please visit
Chris is the CEO of Pinnacle Training & Consulting Systems (PTCS). A continuing education company, that provides educational material in the forms of home study courses, live seminars, DVDs, webinars, articles and min books teaching in-depth, the foundation science, functional assessments and practical application behind Human Movement, that is evidenced based. Chris is both a dynamic physical therapist with 14 years experience, and a personal trainer with 17 years experience, with advanced training, has created over 10 courses, is an experienced international fitness presenter, writes for various websites and international publications, consults and teaches seminars on human movement. For more information, please visit 
 STEP 2: Realize you are an individual
STEP 2: Realize you are an individual