“On the count of three say, ‘CHEESE’!”
The family reunion is captured with a photograph, but grandma (who has Parkinson’s Disease) is not smiling. As a matter of fact, if you didn’t know her you would think she was upset or completely disinterested in the moment. Later, while eating together, the family notices that grandma is drooling while eating and coughing after the meal. When asked if she is ok, her voice is barely above a whisper AND she mumbles, making it difficult to determine if she needs assistance.
What happened to the once smiling, chatty, and boisterous grandma, who was always ready for a fun experience with her family?
Her limited facial expression, trouble with swallowing, and decreased voice volume (hypophonia) are all consequences of the “dark side” of PD.
Parkinson’s Disease is most often characterized by a tremor and/or gait issues. Just as the moon has a dark side, unseen but present, Parkinson’s Disease has a “dark side”, unseen but very present.. As a fitness professional, understanding the “dark side” of Parkinson’s Disease and how it affects your “fighters” will enhance your program design skills, increase your confidence in counseling a “fighter” or care-partner and help build your relationship with other medical and fitness professionals.
The goal of this article series is to shed light on the “dark side” of PD, in the case of this article facial masking, swallowing, vocal issues. By incorporating the knowledge of medical professionals on my “Bridges For Parkinson’s” team, you will learn about research discoveries, resources for program design, useful tools for “fighters” and care-partners and ultimately, hope!
Let’s begin with the Face.
Facial Masking (also known as Hypomimia)
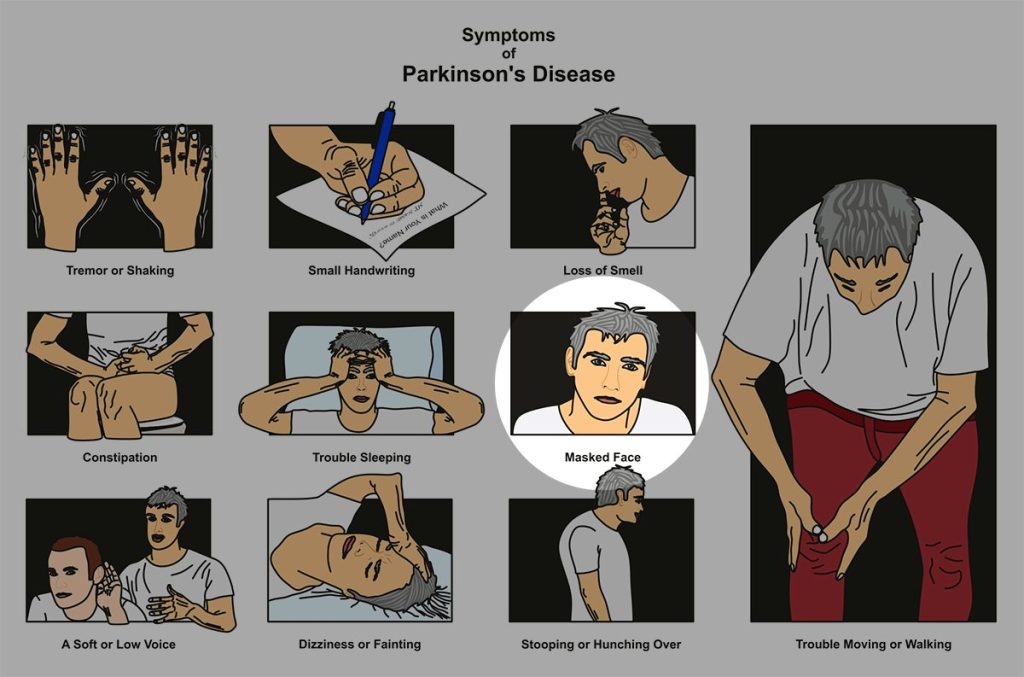
Did you know you have 43 muscles in the face alone? According to the Cleveland Clinic, the craniofacial muscles are “flat muscles that attach to various places on your skull. The craniofacial muscles are essential to chewing and making facial expressions. They originate from bone or fascia and insert into your skin. Craniofacial muscles work together to control movements in your:
- Cheeks
- Chin
- Ears (only in some people)
- Eyebrows
- Eyelids
- Forehead
- Lips (upper and lower)
- Nose and nostrils
Facial muscles are also involved in your unique features, talking, singing, whistling, holding food in the mouth and protecting your eyes.”
Did you know Facial Masking can be categorized into 5 levels? Medical News Today lists the degrees of facial masking as the following.
- 0: normal expression and function
- 1: slight symptoms
- 2: noticeable loss of facial movement
- 3: moderate loss of facial movement, present most of the time
- 4: more severe loss of facial movement or immobilization of the face that is mostly present
- NOTE: research findings show that facial masking is less noticeable during positive interactions while negative interactions produce increased facial masking.
As a fitness professional, ask yourself, if dopamine controls muscle movement, how does lack of dopamine impact those 43 facial muscles?
For people living with PD those muscles are affected, resulting in potential for reduced blinking, lack of eyebrow movement and decreased happy and sad expressions. This can lead those who are unfamiliar with these symptoms to think an individual with PD is upset or apathetic. This couldn’t be further from the truth! They care, but often have no awareness that they are not expressing themselves. They may be unable to communicate effectively while also expressing emotion.
In fact, people suffering from facial masking, hypophonia (low voice volume), and dysphagia (swallowing issues) say the most frustrating part of this experience is isolation. The risk of choking, drooling, or needing to constantly repeat a phrase due to low voice volume is not only exhausting, but may leave them feeling depressed.
Role of Dopamine in the Face
Parkinson’s Disease (PD) is primarily due to the neurodegeneration of dopamine neurons in the substantia nigra, projecting onto the striatum and basal ganglia, which are major movement centers of the brain. These areas act directly on primary motor areas in the cortex to modulate, fine-tune movement and control fast and slow twitch muscles, including facial muscles. However, with the death of dopamine neurons, this signaling tapers off and we see less movement control, often in the form of facial bradykinesia. This can contribute to the effect known as hypomimia, or facial masking, which is thought to be an early sign of PD.

There is no evidence of specific dopaminergic projections that contribute to lack of facial movement currently. However, current research is focused on how lack of dopamine globally triggers facial masking and apathy, especially in early disease states.
Hypomimia, Dysarthria and Tachyphemia (speech) can be debilitating both physiologically and emotionally/socially. Physiologically, having less orofacial movement can impact everyday tasks such as chewing food and swallowing, as there is slower signaling from the basal ganglia modulating motor areas and motor neurons in the muscles (Ricciardi et al., 2020). Socially, facial masking can contribute to a lack of emotional expression and emotional recognition, making it more challenging to interact with loved ones through body language, a discounted but integral part of communication (Wootton et al., 2019).
The addition of dopamine dictates a more robust orofacial response, as often indicated by patients taking dopaminergic medications. A study published in 2020 states that hypomimia was often attenuated by administration of levodopa, hypothesizing that dopamine is involved with voluntary facial expression and emotional recognition (Ricciardi et al., 2020). We could extrapolate this onto other orofacial movements such as swallowing, indicating that these reflexes and severity of hypomimia could come from the decreased dopamine supply. Lack of dopamine affects certain areas of the brain specifically associated with facial expression such as the primary motor cortex and the supplementary motor area, where pathways from the striatum to the cortex project (Makinen et al., 2019). Knowing that the addition of dopamine can help not only with emotional expression but orofacial movements in general may help guide treatment of these debilitating effects, and exercising facial muscles may provide more ease of action when paired with dopamine.
Therapeutics – Medicine and Exercise
Thanks to modern medicine and complementary therapies, addressing facial masking with positive results is possible. Carbidopa-Levadopa is the most prescribed medication for people living with PD. Levodopa enters the brain and helps replace the missing dopamine, which permits people to function better. By increasing the amount of dopamine in the brain, levodopa helps control symptoms and helps you to utilize the facial muscles as well as perform activities of daily living with greater ease.
Physicians may also prescribe dopamine agonists, MAO-Inhibitors and/or COMT- Inhibitors to work with Carbidopa-Levadopa. These medications increase dopamine or additional chemicals in the brain which improves the person’s ability to express emotion and communicate. When combined with exercise, people living with Parkinson’s Disease experience profound improvements.
Research
Complementary therapies such as LSVT LOUD, “Let’s FACE It Together”, and Speech Therapy have been proven to support dopamine replacement therapy. For example;
“Research on LSVT LOUD has documented that people with PD show improvements in loudness and intonation of their speech, as well as clarity of speech, facial expressions.” (LSVT Reference List)
Click here to read part 2 of this article, where we’ll cover tips for fitness professionals…
Co-authored by Colleen Bridges, M. Ed, NSCA-CPT; Renee Rouleau-B.S., PhD student, Jacobs School of Biomedical Sciences, University at Buffalo; Kristi Ramsey, OTD, OTR/L.
References
- ParkinsonsDisease.net (Emily Downward)
- Mayo Clinic
- https://neurologicalsurgery.in/top-facial-exercise-for-parkinsons-patient/
- https://www.mottchildren.org/health-library/hw81637
- https://www.urmc.rochester.edu/encyclopedia/content.aspx?contenttypeid=135&contentid=376
- https://n.neurology.org/content/60/3/432
- Ricciardi, L., De Angelis, A., Marsili, L., Faiman, I., Pradhan, P., Pereira, E. A., Edwards, M. J., Morgante, F., & Bologna, M. (2020). Hypomimia in Parkinson’s disease: an axial sign responsive to levodopa. European Journal of Neurology, 27(12), 2422-2429. https://doi.org/https://doi.org/10.1111/ene.14452
- Mäkinen, E., Joutsa, J., Jaakkola, E., Noponen, T., Johansson, J., Pitkonen, M., Levo, R., Mertsalmi, T., Scheperjans, F., & Kaasinen, V. (2019). Individual parkinsonian motor signs and striatal dopamine transporter deficiency: a study with [I-123]FP-CIT SPECT. Journal of neurology, 266(4), 826–834. https://doi.org/10.1007/s00415-019-09202-6
- Adrienne Wootton, Nicola J. Starkey & Carol C. Barber (2019) Unmoving and unmoved: experiences and consequences of impaired non-verbal expressivity in Parkinson’s patients and their spouses, Disability and Rehabilitation, 41:21, 2516-2527, DOI: 10.1080/09638288.2018.1471166
- National Institute of Diabetes and Digestive and Kidney Diseases. Your digestive system & how it works.
- Finsterer J, Grisold W. Disorders of the lower cranial nerves. J Neurosci Rural Pract. 2015;6(3):377-391. doi:10.4103/0976-3147.158768
- National Institute on Deafness and Other Communication Disorders. Dysphagia.

