Fight Back Stronger! Working with Clients with Parkinson’s Disease
Determined, consistent and tenacious are just a few words I like to use to describe my Parkinson’s Disease “fighters”. I call them “fighters” because instead of lying down and giving up, they have chosen to take charge of their future. They commit to FIGHT BACK against Parkinson’s Disease, and that is a “fight” I want to join!

It is critical that you observe how the “fighter” moves, processes information and responds to challenges. We utilize that information and create fitness programs to address the motor symptoms those living with Parkinson’s Disease (PD) struggle with each and every day.
And the best place to start is with “Foundational Movements” that will broaden a fighter’s Activities of Daily Living (ADL). People living with PD require a unique fitness program to address the impact that PD has on their ADLs.
Foundational Movements
Squats
Lunges
Hinge
Push
Pull
Carry
Rotation
I encourage Fitness Professionals to start with the most basic form of each Foundational Movement before progressing to a more challenging version. Neurologically, progressive and regressive movements make an impact on people living with PD. I have learned that repetition and exercise phases are a necessary part of any fitness program, similar to the human development process.
Consider how humans learn how to move from birth to 3 years of age. First, we learn a skill such as rolling over and we repeat it until we succeed. Then, we move on to unsupported sitting, followed by crawling until one day we are up and running!
And just in case you are wondering, the best place to start with foundational movements is in the warm-up. The repetition of the drills enables the fighters to improve their form, prepare for the work phase and create new neural patterns that will improve their functionality.
Let’s briefly discuss the movement patterns and how each movement can improve ADLs.
Squat
This movement pattern is used daily and assists in maintaining the ability to use synergistic muscular tension, stability and mobility through the torso, hips, knees and ankles. However, every fighter is different which means they will need to start at different levels.
| EXERCISE | ADL |
| Seated knee extension | Toileting |
| Wall Squat | Showering |
| Squat | Dressing |
| Squat/stand and lift heels | Cleaning |
| Squat-jump | Care-giving |
Lunge
Falling or the fear of falling is a significant issue for people living with Parkinson’s Disease. The ability to stand on one leg, shift weight back and forth, maintain an asymmetrical split stance, bend down or get up off the floor is crucial for fall prevention. Lunging, in its various stages, provides Fitness Professionals a way to identify weak links.
NOTE: Some overlap will occur with the lunge and hinge movement.
| EXERCISE | ADL |
| Tap one foot behind | Vacuuming |
| Reverse Lunge | Stepping in/out of shower |
| Step one foot forward | Tying shoelaces |
| Forward lunge | Walking up/down stairs |
Hinge
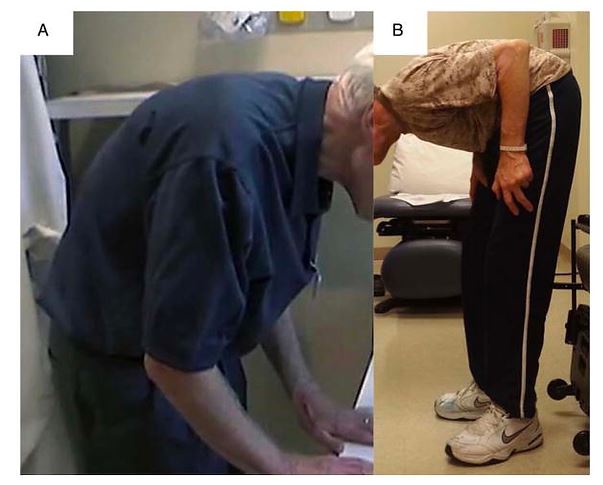
We ALL need to strengthen our posterior chain but it seems to be the one area many Fitness Professionals shy away from including in their program. When you consider how many times a day someone bends over, they must have the strength and basic knowledge of how to hinge so they don’t fall or hurt themselves.
This is even more important for people living with Parkinson’s Disease. If they fall, it could take months for them to recover and by that time, the disease has progressed. Make it a goal to include a hinge movement in every routine.
| EXERCISE | ADL |
| Basic Deadlift with arms crossed | Getting in/out of car |
| Supported Deadlift with one foot behind | Toileting/Showering |
| Traditional Deadlift with weights | Dressing |
| Single Leg Deadlift
Cross-over Deadlift | House and Pet Management |
Push
The push-up is one the most popular exercises of all time! Mastering the “push” is a different challenge. The “push” (not always push-ups) requires core stability, upper back and shoulder strength. Once mastered, people living with PD will notice an increase in power and strength.
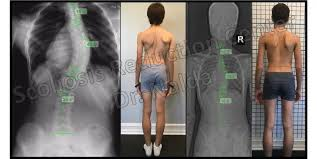
Word of caution: Parkinson’s Disease typically affects a person’s posture. Please remember that anything overhead will alter the center of gravity which means some fighters need to perform a “push” exercise that keeps the arms closer to the body.
| EXERCISE | ADL |
| Wall Push-up | Rising from the floor |
| Push-up on Smith Machine Bar | House cleaning |
| Push-up on knees | Showering |
| Push-up on hands/toes | Pushing large door open |
Pull
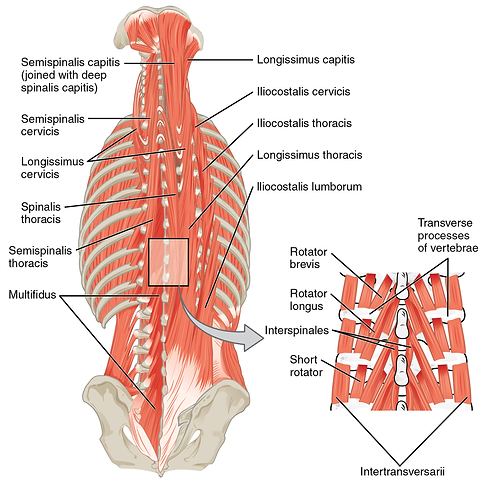
With so many postural issues due to weak muscles, developing a stronger “pull” will help people living with PD strengthen their back muscles which will decrease falls, improve posture and relieve back pain.
| EXERCISE | ADL |
| Shoulder retraction only | Opening refrigerator |
| Shoulder retraction and hold | Vacuuming/sweeping |
| “Row” arms (no weights) | Showering |
| “Row” with tubes | Pulling up pants |
| “Row” with one arm | Picking a child or pet up |
Carry
People living with PD want the ability to carry a grocery bag, walk and pull out keys all at the same time. But if they do not know how to use their body correctly, multitasking can be scary. Carry exercises focus on leverage and load. The good thing is we can always make adjustments depending on other variables. For example, bad shoulders mitigate against the overhead version of the carry while weak hands prevent one from carrying heavy loads. Carry exercises don’t necessarily help prevent falling other than the benefits they provide by strengthening the core. However, Fitness Professionals need to remember that carry exercises will serve your fighters in the early pre-kyphosis stage as a posture exercise. Carry exercises also provide a challenging asymmetrical exercise if performed unilaterally.
TIP: The carry movement is a great way to challenge the core without doing crunches!
However, before beginning a gait/carry movement with your fighters, make sure they have been thoroughly assessed.
| EXERCISE | ADL |
| Walking | Carrying groceries |
| Bird dog walk | Carrying laundry basket |
| Farmer’s walk with two weights | Child care |
| Farmer’s walk with one weight | Pet Care |
| Farmer’s walk with one weight overhead | House Management |
Rotation
The core maintains the stability and strength of the torso and acts as a conduit for energy. The movement patterns listed above encourage core strength which means rotational exercises are not so much a movement pattern as a powerful supplement to the above foundational movements.
Rotational exercises for people living with PD help improve gait and posture, reduce falls, improve coordination and mobility, increase overall strength and, most importantly, enable them to independently perform ADLs.
Rotation Reminders for Fitness Professionals:
- Torso stabilizes the spine and allows movement by coordinating with the pelvic muscles.
- Flex, extend, bend and rotate
- Anti-Rotational Exercises best for beginners. People living with Parkinson’s DIsease often deal with Processing Information issues. Begin with basic exercises in order for fighters to learn proper form and technique.
- Muscles – Rectus Abdominis, obliques, rhomboids, deltoids, glutes, abductors, quads and adductors
Caution! Be sure to include the hips and the lower portion of the spine when rotating.
| EXERCISE | ADL |
| Isometric tube hold | Enter/exit tub or shower |
| Isometric tube hold and step laterally | Enter/exit vehicle |
| Circles with tube | Emptying dishwasher |
| Circles with tube/squat | Laundry related activities |
| Torso rotation with tube | All ADL categories |
In closing, when Fitness Professionals learn the art of organizing movement patterns and creating a program that uses these foundational movements, their fighters living with Parkinson’s Disease experience physical gains such as standing without support, joint mobility, active core stabilization, integrated joint action, cognitive improvement and most importantly the ability to handle a challenging moment with confidence.
Having acquired these foundational skills with the help of you, their Fitness Professional, build trust and credibility for supporting a fighter’s long-term commitment to HOPE. As noted at the beginning of this article, our fighters are determined, consistent and tenacious. They have chosen to take charge of their future and FIGHT BACK against Parkinson’s Disease — a “fight” I hope you, as a Fitness Professional, join!
Become a Parkinson’s Fitness Specialist
You can acquire the tools and resources necessary to integrate foundational movements with ADLs within the Parkinson’s community. Sign up for Colleen’s 12.5-hour online course on MedFit Classroom, Parkinson’s Disease Fitness Specialist.
Colleen Bridges has worked for nearly 17 years as an NSCA Certified personal trainer, group exercise instructor and fitness consultant and as an independent contractor for Nashville’s first personal training center, STEPS Fitness. Her passion for understanding the body in sickness and in health, and how it moves, as fed her interest in and enhanced her talent for working with senior adults, especially those living with a neurological disorder such as Parkinson’s Disease.