5 Pilates Exercises to Improve Respiratory Function
Pilates is a total body exercise method that is highly effective for strengthening and lengthening the entire body. While Pilates is mostly known to improve core strength (the “Powerhouse”), posture, and range of motion, this exercise method can be used to improve respiratory function in those suffering from respiratory diseases. Respiratory diseases include asthma, COPD, chronic bronchitis, emphysema, lung cancer, cystic fibrosis, pneumonia, and now COVID-19. These diseases affect the way one breathes and lowers oxygen saturation that the body needs to function properly. One of the main principles in Pilates is breathing, thus the need to take a closer look at the effects of Pilates on respiratory function.
Benefits of Pilates Related to Respiratory Disease
- Improves postural cavity to breathe properly.
- Expands breathing capacity with diaphragmatic breathing.
- Increases pulmonary ventilation which is needed for better respiratory function.
- Improves lung volume.
- Develops intercostal muscles (respiratory muscles) to better “squeeze” out impure air.
- Improves exhaling all impure air out of the body while inhaling pure air.
- Improves thoracoabdominal mobility.
- Improves circulation to deliver oxygenated blood more efficiently.
- Increased SpO2 (blood oxygen saturation).
- >95% indicates healthy respiratory function.
- <95% indicates taxed respiratory function.
The Pilates Breathing Method
Joseph Pilates, the creator of Contrology, stated in his book Return to Life Through Contrology: “Lazy breathing converts the lungs, literally and figuratively speaking, into a cemetery for the deposition of diseased, dying and dead germs as well as supplying an ideal haven for the multiplication of other harmful germs.”1
- Lateral Breathing: The main goal for Pilates breathing is to breathe deeply expanding the ribcage without raising the abdominal muscles training them to jet out. Therefore, deep lateral breathing through the ribcage is the hub of the breathing technique. Proper breathing is inhaling through the nose and exhaling forcefully through the mouth. When one inhales, the ribcage expands out to the sides using the intercostal muscles, and then when exhaling the ribcage knits together like one is being sinched in a corset. According to Joseph Pilates, one should exhale forcefully getting all impure air out of the lungs like wringing out every drop of water out of a wet cloth.
- Set Breathing Pattern: When performing the Pilates exercises, one should inhale to prep for the movement and exhale as one performs the movement.
- Rhythmic Breathing Pattern: In some exercises, one breathes in rhythm to the exercise. This breathing consciously activates respiratory muscles to enable the lungs to expand and transport oxygen.
5 Effective Pilates Exercises to Improve Respiratory Function
The Hundred (Rhythmic Breathing)
- Begin a tabletop position with the shoulder blades and head lifted off the mat looking forward.
- Pump the arms up and down 100 times vigorously so the abdominals respond to and control the movement.
- Inhale through the nose 5 times to the rhythm of the arms pumping, then exhale 5 times to the rhythm of the arms pumping.
- Keep the lower back imprinted to the mat at all times.

Single Leg Stretch (Rhythmic Breathing)
- In a supine position, lift the shoulder blades and head off the mat looking forward.
- Bend the right knee towards the chest as the left leg extends straight out hovering over the mat.
- Inhale through the nose as you switch the legs 2 times, then exhale as you switch the legs 2 times.
- Inhale, inhale, exhale, exhale as you switch, switch, switch, switch.
- Keep the lower back imprinted to the mat at all times.
- Perform 8 sets.
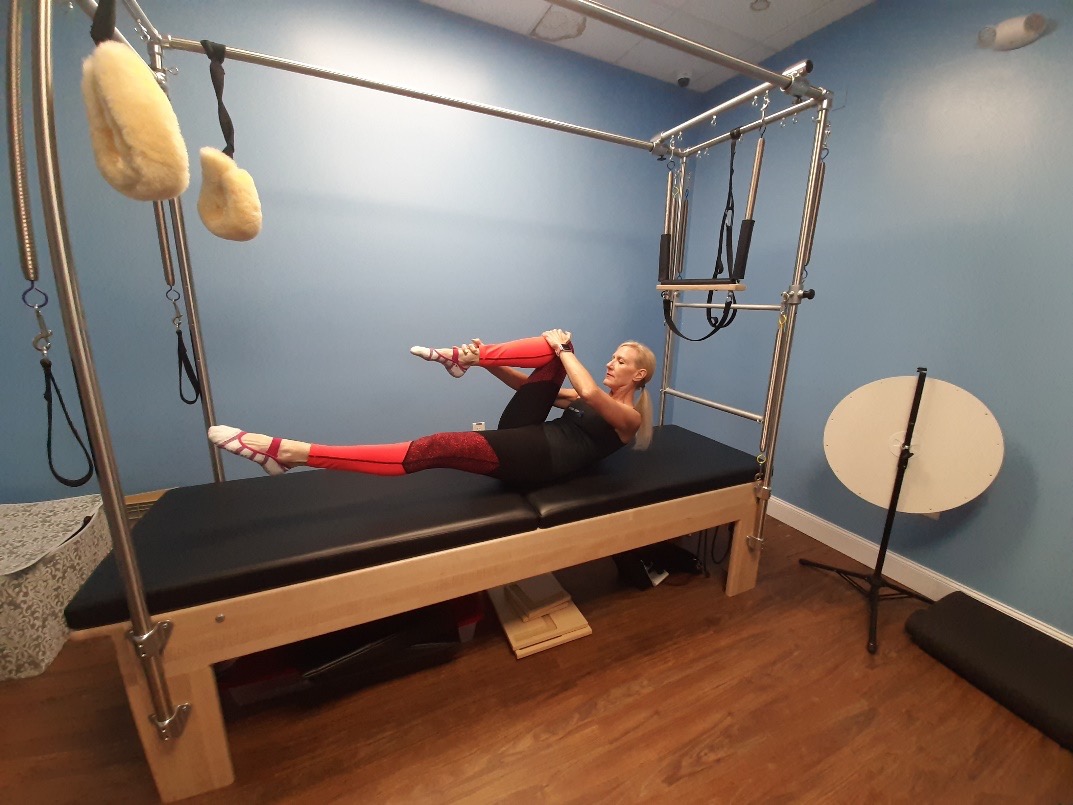
Dying Bug (Set Breathing Pattern)
- In a supine position, position the legs in table-top and arms extend straight up towards the ceiling.
- Press the right hand firmly on the right thigh and press the right thigh to the right hand in opposition.
- Inhale through the nose as you extend the left arm back overhead and the left leg extends straight out hovering over the mat.
- Exhale through the mouth and draw the arm in and the leg back to tabletop. Repeat on same side and switch.
- Keep the lower back imprinted to the mat at all times.
- Perform 8 reps on each side.

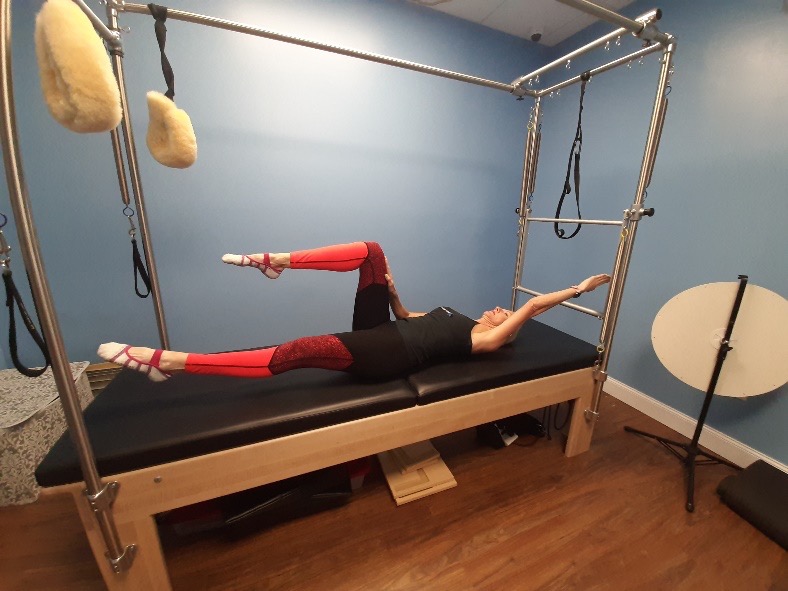
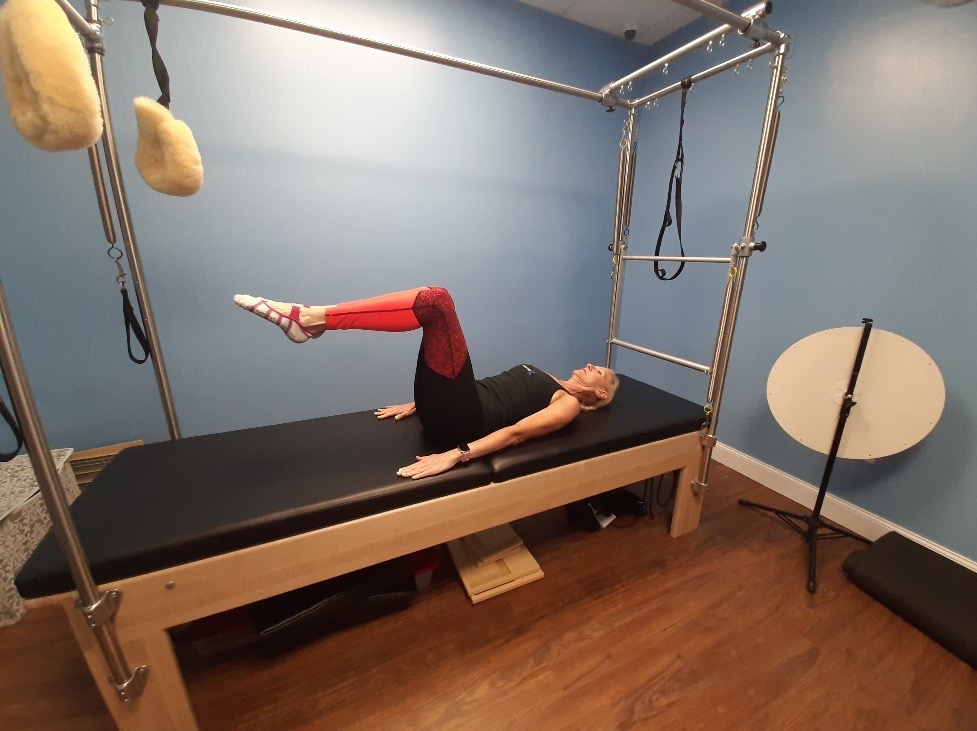
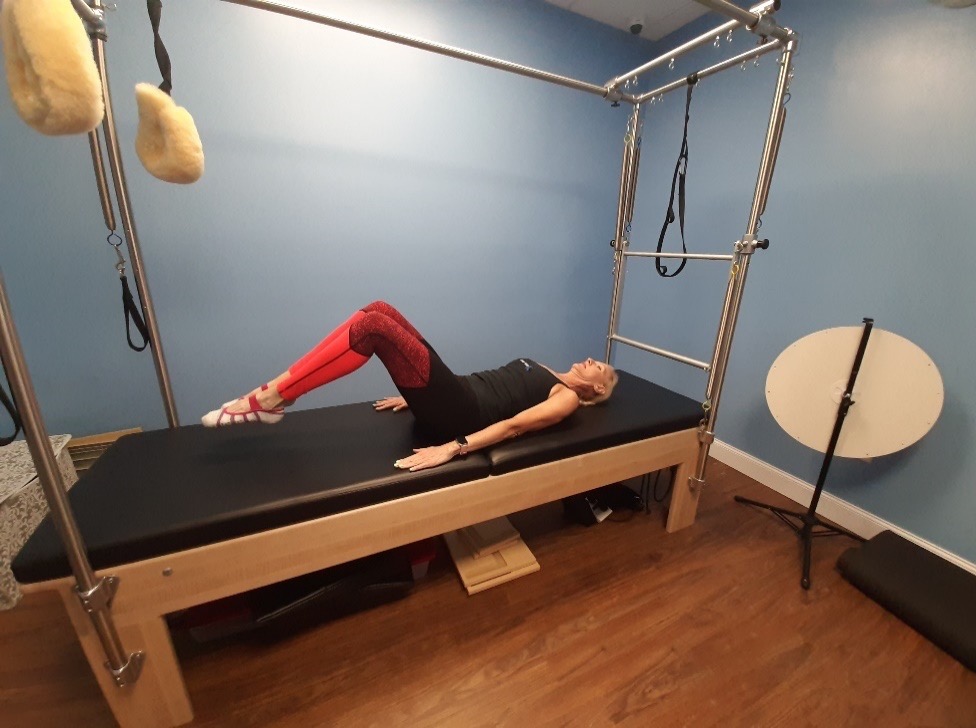
Toe Taps (Set Breathing Pattern)
- In a supine position, lift the legs into tabletop keeping the upper body and head down on the mat.
- Anker the arms next to the body pulling the shoulders back and down on the mat.
- Inhale through the nose as you lower both feet and legs together towards the mat. Keep the knees at 90º and the feet away from the glutes.
- Exhale as you pull the legs back up to tabletop.
- Keep the lower back imprinted to the mat at all times.
- Perform 10 reps.
Thread the Needle (Set Breathing Pattern)
- Start in a side kneeling position with the hips lifted off the mat and one forearm down on the mat with the other arm straight up to the ceiling.
- Inhale through the nose as you lean the body back an inch to expand the ribcage.
- Exhale through the mouth as you rotate forward and thread the arm under the armpit towards the back. Crunch the obliques and transverse abs.
- Inhale through the nose as you un-rotate and return to the start position with the arm lifted towards the ceiling.
- Perform 8 reps on each side.


Pilates, respiratory function and research
The literature is scarce and sometimes conflicting about the benefits of Pilates breathing related to the respiratory system. However, there are some existing studies that look at the increase in lung volumes, respiratory motion, SpO2, and the reduction in respiratory rate using Pilates breathing exercises. More research needs to be conducted. Refer to suggested reading at bottom of article.
Education for Fit Pros
Fitness Professionals & Personal Trainers: Become a Respiratory Disease Fitness Specialist!
Some of your clients may suffer from a respiratory disease and you may be an important source of relief. The Respiratory Disease Fitness Specialist online course will equip you with the knowledge to safely and effectively work with these clients to help improve their quality of life.

CarolAnn, M.S. Exercise Science and Health Promotion, is a 30+ year veteran in the fitness industry educating other health/fitness professionals to increase their expertise and brand influence. She is on the MedFit Education Advisory Board and the head health/fitness educator for FiTOUR. She is currently the Head Instructor at Club Pilates in Athens, GA.
Suggested Reading
- Cancelliero-Gaiad, K. M., Ike, D., Pantoni, C. B., Borghi-Silva, A., & Costa, D. (2014). Respiratory pattern of diaphragmatic breathing and pilates breathing in COPD subjects. Brazilian journal of physical therapy, 18(4), 291– https://doi.org/10.1590/bjpt-rbf.2014.0042
- de Jesus, L.T., Baltieri, L., de Oliveira, L.G., Angeli, L.R., Antonio, S.P., Pazzianotto-Fort, E.M. (2015) Effects of the Pilates method on lung function, thoracoabdominal mobility and respiratory muscle strength: non-randomized placebo-controlled clinical trial. Pesqui. vol.22 no.3. http://www.scielo.br/scielo.php?pid=S1809-29502015000300213&script=sci_arttext&tlng=en
- Hagag, A.A., Salem, E.Y. (2019) Pilates Exercises Improve Postural Stability, Ventilatory Functions and Functional Capacity in Patients with Chronic Obstructive Pulmonary Disease. IOSR Journal of Nursing and Health Science (IOSR-JNHS), vol. 8, Issue 4 Ser. VI., PP 86-91 http://iosrjournals.org/iosr-jnhs/papers/vol8-issue4/Series-6/M0804068691.pdf
- Baglan Yentur S, Saraç DC, Sarİ F, et al. (2020). Fri0613-hpr the effects of pilates training on respiratory muscle strenght in patients with ankylosing spondylitis. Annals of the Rheumatic Diseases;79:912. http://dx.doi.org/10.1136/annrheumdis-2020-eular.2129
References
- Pilates, J., William, J. M., Gallagher, S., Kryzanowska, R. (2000). The Complete Writings of Joseph H. Pilates: Return to Life Through Contrology and Your Health. BainBridge Books, Philadelphia, PA. (Originally written 1945)