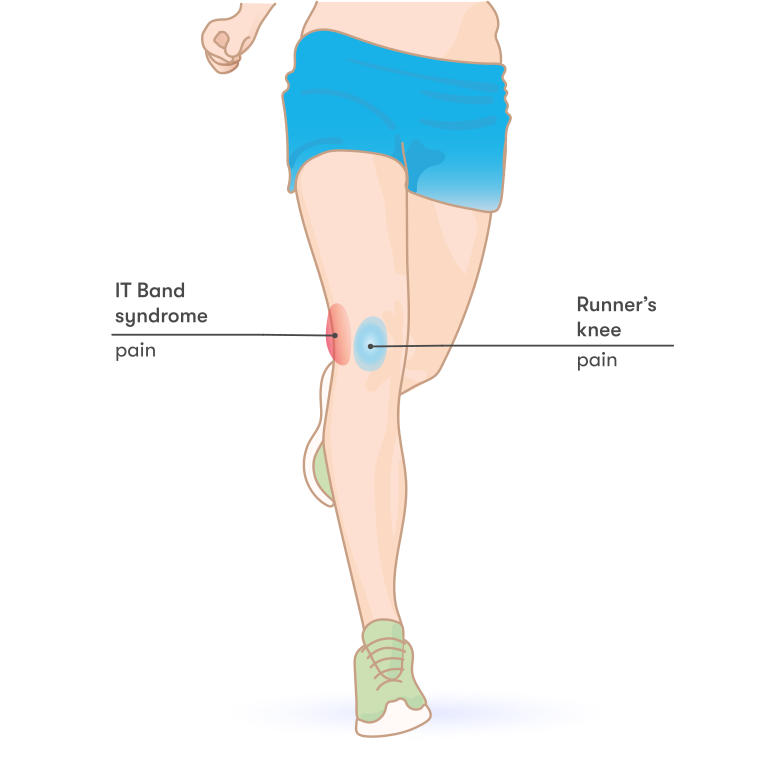
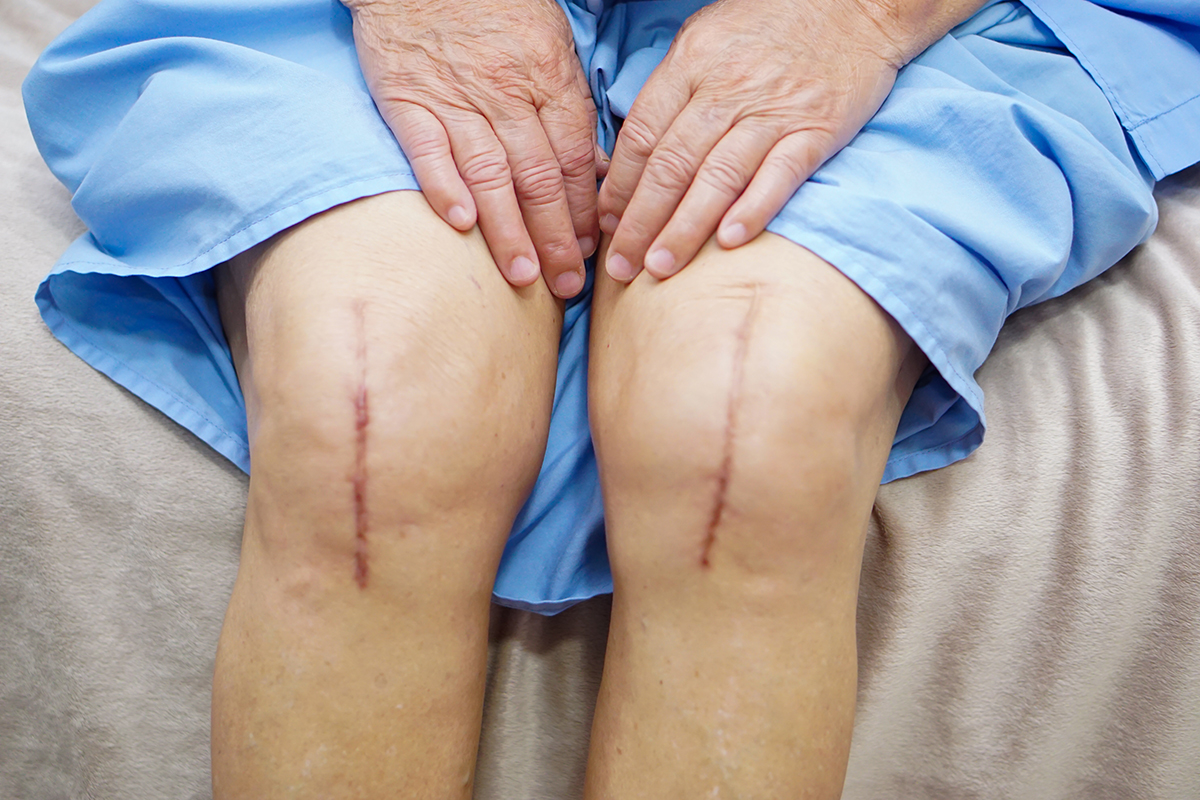
Don’t Let Arthritis Stop You: Move On
Arthritis comes in many forms and has many manifestations, affecting almost every joint in the body. We generally speak in terms of the two most-known if not popular forms of arthritis: rheumatoid (RA) and osteo-arthritis (OA.) The essential difference is in the root cause. RA is an auto-immune disease whereby the body, for unknown reasons, attacks itself, particularly in the joints. OA, on the other hand, is often considered the downstream effect of wear and tear, over-use, prior injury, or, as we’re seeing more of as society gets more sedentary, from lack of use. In OA, typically, some insult to the joint disrupts the natural repair processes and further deterioration occurs subsequently.
Due to their differing causes, there are obviously differing treatments; but the basics of medical management are essentially the same. I am not qualified to address the specifics of the treatments available but, in lay terms, treatment usually entails some version of anti-inflammation and pain-reduction drugs, precautionary movement or positional guidance (don’t do’s, for example), physical therapy to manage pain and inflammation, and therapeutic exercises to support the structures affected as the disease itself causes not just inflammation and pain but damage to the structures that support the joints. Typically we identify arthritis as something that damages cartilage and, in truth, that is often what the standard ‘films’ – X-ray, possibly MRI (magnetic resonance imaging) – show. We now know that the synovial sacs around the joint are also affected and that these and other chemical disturbances affect the muscles and tendons that move and support the joint. In almost all cases of arthritis, pain, inflammation, reduced strength and range of motion (ROM) ensue, diminishing quality of life in many ways and, because some of the drugs used to treat it, potentially reducing quantity of life. (Gastrointestinal bleeding from non-steroidal anti-inflammatories (NSAIDs) or bone loss (osteoporosis) from corticosteroids can lead to fatal outcomes (such as spontaneous fractures leading to falls from osteoporosis) if not treated with other medications.)
When someone is potentially afflicted or actually diagnosed with a form of arthritis, the medical community goes into hyper-drive, encouraging changing one’s habits, be they the types of activities one engages in recreational, competitively, or professionally; or the types of non-activities one currently does, in particular, being inactive.
In some cases, dietary advice is offered as we are learning more about foods that are pro-inflammatory and others that have anti-inflammatory benefits. In the former category, we are learning that excessive sugar or simple carbohydrates, including processed wheat products, may exacerbate inflammation while others, such as salmon, dark, green veggies, and certain oils (e.g., olive oil) are capable of reducing the inflammatory elements circulating throughout our bodies and our joints. Furthermore, in more extreme cases, when arthritis becomes very painful and debilitating, over-the-counter and/or prescription-fitted braces may be offered to defer some of the more end-line procedures such as surgery to fuse the joint or replace it with a prosthetic device.
The most common non-pharmaceutical and non-surgical treatment for arthritis of any sort: exercise.
Note that there are several legitimate ways to integrate exercise through resistance training programs that have proven quite effective in arthritis management. Yoga, Pilates (floor or machine based), Tai Chi, Qigong and water-based, or aqua, exercise are all beneficial to many aspects of the overall arthritis program of strength, ROM, proprioception and ultimately function. Since many of these are quite technical and are often done in class formats, one should ask the instructor(s) as to their experience working with arthritis clients.
As with any form of exercise, by whatever professional instruction, you should be totally aware of your pain levels as going “through” the pain is not recommended; thus, you must assert control over the exercise sessions. There will be some exercises, however, that are not destructive and may be somewhat painful but must be done in order to maintain reasonable levels of function and independence. So long as the pain subsides within a couple of hours – preferably as soon as you stop – and there is no exacerbation of inflammation the next day, you can assume that the exercise was just enough. If symptoms flare up over the next 24 hours, however, assume you did more than you should have and alert your trainer or instructor so that he/she can avoid doing the aggravating exercise(s) as much or as hard next time. For these reasons, along with all the other recommendations so far as exercise interventions are concerned, it is best to seek the counsel and assistance of a fitness professional with a background in medical fitness. This could be someone with a more advanced academic degree, someone with a license to practice rehabilitation exercise (physical therapist, athletic trainer, etc.), or someone who’s taken several educational programs to have a greater understanding of the variety of disorders and diseases that may benefit from exercise interventions.
UPCOMING WEBINAR
Dr. Irv Rubenstein graduated Vanderbilt-Peabody in 1988 with a PhD in exercise science, having already co-founded STEPS Fitness, Inc. two years earlier — Tennessee’s first personal fitness training center. One of his goals was to foster the evolution of the then-fledgling field of personal training into a viable and mature profession, and has done so over the past 3 decades, teaching trainers across through country. As a writer and speaker, Dr. Irv has earned a national reputation as one who can answer the hard questions about exercise and fitness – not just the “how” but the “why”.