Can Mindfulness Improve your Balance?
Short answer: Absolutely.
Focused attention has the power to improve your health, mood and cognition. When it comes to moving steadier, research shows that practicing mindfulness while walking can improve balance in older adults. This is a simple practice that anyone can do to move more freely and live more fully with more confidence.

What is Mindfulness?
Being mindful means to simply focus on the present moment. Its roots stem from ancient eastern and Buddhist philosophy. It includes being aware of your thoughts, feelings, sensations and the surrounding environment through a gentle, nurturing lens. This way you can tune into what you are sensing in the present moment rather than living in and rehashing the past or projecting into the future.
Mindfulness Elevates Health
Do a PubMed search on “mindfulness and health” and 14,955 studies pop up in the National Library of Medicine! These research studies show there are numerous well-being benefits that can help people of any age with any health condition including:
- Reducing stress and pain
- Improving physical health and chronic conditions like arthritis, diabetes and cancer
- Promoting cognitive function, attention and memory
- Elevating emotional well-being and mood
- Healthier aging and resilience
- Improving balance!
One foundational way that mindfulness and meditation improve health is by calming your nervous system. Moving out of the sympathetic stress response and into the parasympathetic relaxation response is where health happens. It’s where the body can rest, digest, heal and repair itself.
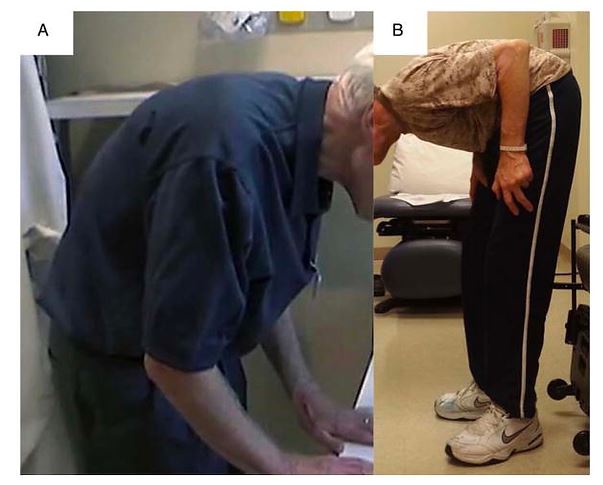
Constantly living in “stress mode” where you always feel overwhelmed, fearful or tense puts your body into a chronic state of inflammation that damages cells, tissues and organs. This damage accumulates and can lead to impaired bodily systems from your nervous system, respiratory, cardiovascular, musculoskeletal, and immune system. This can result in inflammaging where the body is under constant stress and strain and breaks down more than it can repair itself. It is a major reason for the age-related decline in physical and cognitive function that makes it more difficult to move and think smoothly and easily.
Mindfulness for Better Balance
It’s well-accepted that practicing Tai Chi improves ankle proprioception and balance. Now studies are showing that walking meditation can do the same for elderly women and older adults with history of falling (1, 2). Walking meditation has even been shown to improve ankle proprioception and balance performance in people with chronic ankle instability! (3)
Walking meditation is a mindfulness practice where you walk slowly while focusing your attention on your leg and foot movements (2). Researchers saw improved ankle proprioception and balance improvements with older adults being able to stand on one leg for a longer time as well as increased neuromuscular control. When focusing your attention on your movement, researchers think that this improves the brain processes related to body awareness and balance adjustments (1).
Stronger neural and muscular connections mean you can be faster to sense and respond to your everyday environment, as well as recover from the loss of balance to effectively prevent a life changing injury or fall.
Practice Mindful Movement
For the happiest, healthiest and safest holiday season, before engaging in activity, focus on “BEAM” to relieve stress, boost mood, build a sharper brain, taller posture and better balance. BEAM is an acronym that stands for Breathe, Elongate, Align and Move Mindfully.
You can imagine being as long, strong and sturdy as a “beam.” Another meaning of “beam” is to be happy, smiling and radiating a line of bright light or energy. Visualizations can enhance physical and emotional well-being and help bring your attention into the present moment.
BEAM for Better Brain, Body and Balance
Breathe: take 3-4 deep breaths into the front, back and sides of your belly, up into your ribs and then chest; exhale in the opposite direction from your chest, ribs and then squeeze your belly button towards your spine.
Elongate: lengthen your spine on each inhalation lifting from the crown of your head
Align your body: feel light with body parts lined up; ears over shoulders, shoulders over hips, hips over knees and ankles. Practice standing with feet hip distance apart, toes pointing forward and knees softly bending over your second and third toes; pelvis is in neutral, your sternum lifts up and out with ribs aligned over pelvis, shoulders are back and down away from the ears, line up ears over shoulders that are over hips, knees and ankles.
Move Mindfully: think about where you are and what you are about to do; whether you are cooking, cleaning, going up or down stairs or walking inside or outside focus on your leg and foot movements
Practice BEAMing throughout your day so you can move mindfully and enjoy feeling sharper, steadier, lighter and more confident with each step you take throughout the holiday season.
Fit Pros: Guide Older Clients as a Geriatric Fitness and Lifestyle Specialist
Millions of people over age 65 looking for guidance from fitness professionals who are knowledgeable in exercise, nutrition and lifestyle principles that can help them improve functional mobility, while also preventing and managing chronic conditions to live their highest quality of life. The Geriatric Fitness and Lifestyle Specialist online certificate course will give you insights, strategies and tools to be a successful professional in this rapidly growing market. Learn how to be a valued part of clients’ continuum of care, working with the medical team to improve functional outcomes and positively impact people’s lives.

Cate Reade, MS, RD is a Registered Dietitian and Exercise Physiologist on a mission to improve functional mobility and health span utilizing the power of lifestyle medicine. She has been teaching, writing and prescribing healthy eating and exercise programs for over 25 years. Today, as CEO of Resistance Dynamics and inventor of the MoveMor™ Mobility Trainer, she develops exercise products and programs that target joint flexibility, strength and balance deficits to help older adults fall less and live more.
References
- https://pubmed.ncbi.nlm.nih.gov/31563384/. Walking meditation promotes ankle proprioception and balance performance among elderly women.” Jour Bodywork & Movement Therapies 2019
- https://pubmed.ncbi.nlm.nih.gov/34931904/. “Walking meditation versus balance training for improving balance abilities among older adults with history of fall: A randomized controlled trial.” Clin Rehabil. 2022
- https://europepmc.org/article/med/35093512. Comparative effect of walking meditation and rubber-band exercise on ankle proprioception and balance performance among persons with chronic ankle instability: A randomized controlled trial. Europe PMC 2022